Viruses we don't test for
A brief guide to the respiratory pathogens flying under the radar
Force is growing, and so is the team. I'm excited to welcome Gage Moreno, PhD, as a contributing writer. Like our upcoming move to a standalone website, expanding the team is part of the plan to make this publication more valuable to you over the long term. This is the first explainer in a two-part series; Part II will cover how epidemiologists track these pathogens, and what future technologies might improve surveillance. -Caitlin
If you’ve ever been sick with “a cold,” yet tested negative for flu and Covid-19, you’ve already bumped up against a hidden world of viruses.
“A cold” isn’t a single illness it’s a label used for dozens of respiratory pathogens that circulate every year, most of which are rarely tested for. Even though they are largely invisible to patients, these viruses cause real illness, drive outbreaks, and shape seasonal patterns.
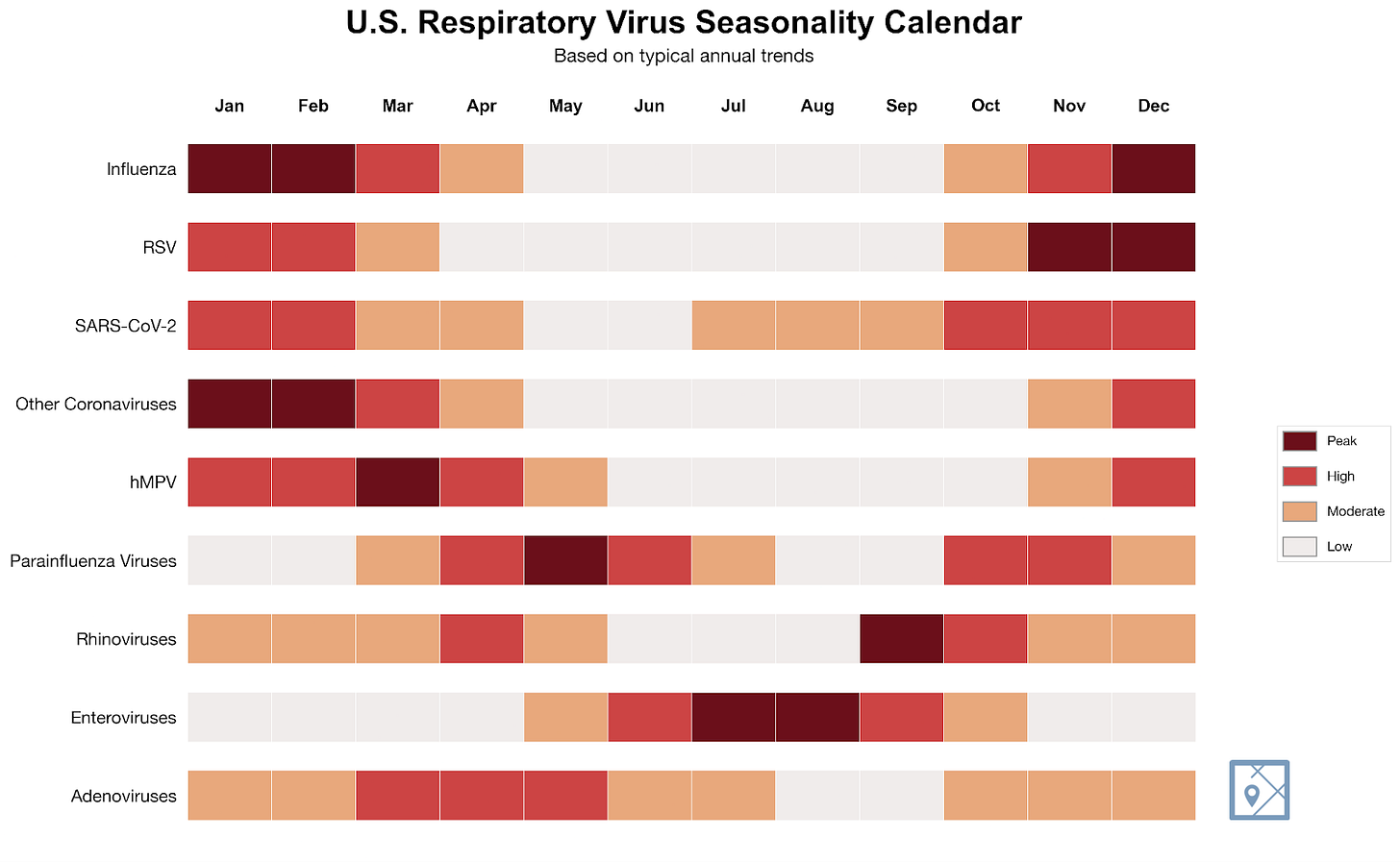
What follows is a short primer on some of the more common but under-recognized respiratory viruses. These are viruses that epidemiologists track and clinicians recognize, but most people have never heard of by name.
What’s out there
Adenovirus
Adenoviruses are a large and diverse group of viruses. Over 100 types have been identified, 49 of which can infect humans, spanning seven major species (named A–G). They can cause respiratory illness, conjunctivitis, and gastrointestinal symptoms. In the respiratory context, infections often present with fever, sore throat, cough, and sometimes pink eye, an unusual but distinctive combination.
Most infections are mild, but certain types of adenovirus can cause more severe disease, particularly in young children and people who are immunocompromised. Since late 2021, there have been rare clusters of acute severe hepatitis in children that were not caused by hepatitis A–E viruses, and many of these cases have been linked to human adenovirus infection, particularly type 41.
Transmission occurs primarily through respiratory droplets and contact with contaminated surfaces. The virus is notably hardy in the environment, which helps explain why it can spread efficiently in close-contact settings.
One interesting fact: the U.S. military vaccinates recruits against specific adenovirus types (4 and 7) because of historically large outbreaks in training and other congregate settings. The vaccine is used in the military because recruits live and train in very close quarters, where adenovirus can spread rapidly and cause large, disruptive outbreaks. It is a live oral vaccine, so it is not suitable for people with weakened immune systems. In most healthy civilians, infections are mild, so routine vaccination outside that high-risk setting isn’t needed.
Human metapneumovirus
Human metapneumovirus (hMPV) was only discovered in 2001, but it is now known to circulate widely. It’s a cousin of RSV and causes similar symptoms as adenovirus: cough, fever, congestion, and sometimes wheezing or shortness of breath.
It spreads through respiratory droplets and close contact, peaking in late winter to spring. In healthy adults, infection is usually mild, but young children, older adults, and people with weakened immune systems can develop more serious illness, including wheezing or asthma flare-ups, ear infections, bronchiolitis or pneumonia, and the distinctive “barking” cough of croup. People can get hMPV multiple times in their lives, with repeated infections usually being milder.
Because of their close genetic relationship, researchers have been exploring ways to protect against both hMPV and RSV. A few studies have described monoclonal antibodies capable of neutralizing both viruses, but currently approved monoclonal treatments target only RSV. These findings point to the potential for future therapies that could provide broader protection against multiple respiratory viruses in vulnerable populations.
Parainfluenza viruses
Despite the name, human parainfluenza viruses (HPIVs) are not closely related to influenza viruses. They are a group of four viruses that commonly infect children but they do also circulate in adults.
HPIVs typically cause symptoms similar to other respiratory viruses: cough, sore throat, and congestion. Severe disease is more common in young children, who can develop croup, bronchiolitis, bronchitis, or pneumonia. These infections may also worsen underlying lung conditions such as asthma. Symptoms of more serious illness in children can include a barking cough, hoarseness, stridor, and wheezing.
In adults, severe parainfluenza infections are less common but can lead to bronchitis or pneumonia, especially in older adults or those with weakened immune systems. Transmission occurs through respiratory droplets and contaminated surfaces, and different types circulate at different times of year, contributing to a steady background of respiratory illness outside of flu season.
Common human coronaviruses
Before Covid-19, several human coronaviruses were already circulating globally, including OC43, 229E, NL63, and HKU1. They are a common cause of mild respiratory illness, often referred to as “the common cold.” Some of these, like NL63 and HKU1, were only identified in the early 2000s, though genetic analyses suggest they have been circulating in humans for decades prior.
In healthy adults, infection typically causes runny nose, cough, sore throat, and low-grade fever. Most people experience repeated infections throughout life, usually with milder symptoms each time.
In infants, young children, older adults, and people with weakened immune systems, these viruses can occasionally cause more serious lower respiratory illness, including bronchiolitis or pneumonia. While severe cases are uncommon, immunocompromised adults may experience prolonged symptoms or complications from these otherwise mild viruses.
Transmission occurs through respiratory droplets and close contact, and activity tends to peak in the winter months.
Rhino/Enteroviruses
Rhinoviruses and enteroviruses are part of the same large viral family, Picornaviridae, and include hundreds of types. Rhinoviruses are grouped into three species (A, B, and C), while enteroviruses span multiple species (A-D), including well-known types like coxsackieviruses, echoviruses, and poliovirus. Because of their genetic similarity, they are often grouped together in diagnostic testing as “rhino/enterovirus.”
Most infections look like a standard cold: runny nose, cough, sore throat, and sometimes fever. Rhinoviruses are the leading cause of the “common cold,” while enteroviruses can also cause illnesses like hand, foot, and mouth disease. Because enteroviruses replicate in the gastrointestinal tract, some infections can cause mild stomach symptoms such as nausea, vomiting, or abdominal discomfort, though they are not the main cause of classic stomach bugs.
This group also includes viruses with a wider range of clinical outcomes. Enteroviruses are closely related to poliovirus, and while paralytic disease is now rare, some types can still cause more serious complications. For example, EV-D68 has been associated with rare cases of a polio-like illness called acute flaccid myelitis, and both rhinoviruses and enteroviruses can trigger asthma exacerbations or more serious respiratory illness in vulnerable populations.
These viruses are extremely common in the community, so children are exposed frequently. Young children can experience multiple rhinovirus infections each year, often six to eight, and by adulthood, most people have been exposed to dozens of rhinovirus and enterovirus types. Immunity is partial and often short-lived, so repeated infections occur throughout life, which is why colds and other mild infections continue even in adults.
Because there are so many types and immunity is incomplete, rhinoviruses and enteroviruses circulate year-round, with peaks in the fall and spring.
Prevention
If you’re a parent facing the first year of daycare, you’ll know that kids are constantly sick. Each cold or mild infection is frequently a first encounter with a new virus, so their immune systems are constantly learning and responding.
Prevention for all of these viruses is familiar because they spread in similar ways. Good ventilation, staying home when sick, and basic hand hygiene all help reduce transmission.
High-quality masks, like KN95s, are also effective, especially in high-risk settings or during periods of high respiratory virus activity. Masks not only protect the wearer but also help prevent viruses from spreading to others, making them a powerful tool for reducing transmission in the community.
Gage Moreno, PhD, is a genomic epidemiologist who uses large-scale sequencing data to study respiratory virus transmission, focusing on how pathogens spread through communities and how we detect them.




Lots of interest in refining mode of transmission info, e.g., droplet vs aerosol. I will put that on the list of things we can look into and write about.
Improving indoor air quality isn't expensive or difficult. HVAC systems can upgrade to MERV13 filters elements, install in-duct UV-C disinfecting lights, increase outside air exchanges, portable HEPA filter units can be used for localized air treatment around infected individuals. The key is to get it codified in building codes.